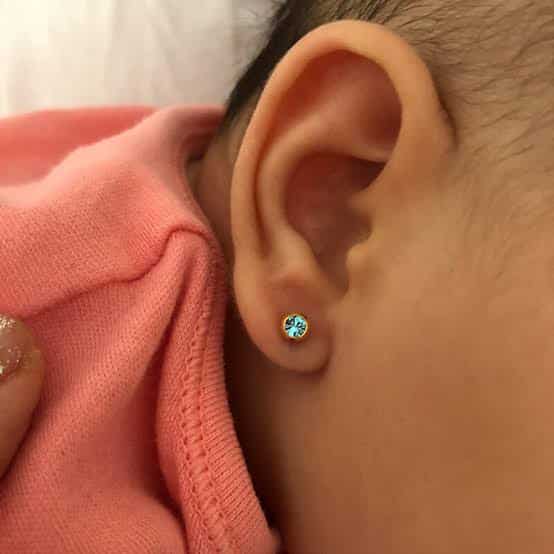
Ear piercing in children is a personal decision for parents, but there are several important factors to consider before going ahead. Here’s what you need to know:
1. Best Age for Ear Piercing
- The American Academy of Pediatrics (AAP) states that ear piercing is safe at any age if done properly. However, they recommend waiting until the child is old enough to care for the piercings themselves (usually around 6–8 years old) to reduce the risk of infection.
- Some parents choose to pierce their baby’s ears early (as young as a few months old) because infants tend to heal faster and are less likely to touch or pull on their earrings.
2. Choosing a Safe Piercing Method
- Needle vs. Piercing Gun: Professional piercers often recommend a needle over a gun because it’s more sterile, precise, and causes less trauma to the ear. Piercing guns can create more tissue damage and are harder to sterilize.
- Go to a Licensed Professional: Ensure the piercing is done by a trained professional in a clean and reputable setting. Many pediatricians also offer ear piercing.
3. Choosing the Right Earrings
- Use hypoallergenic metals such as surgical steel, titanium, or 14K+ gold to reduce the risk of allergic reactions.
- Avoid earrings with nickel, as it can cause irritation.
- Opt for small, flat-back earrings to prevent snagging.
4. Caring for Newly Pierced Ears
- Clean twice a day with saline solution or antiseptic recommended by the piercer. Avoid using alcohol or hydrogen peroxide, as they can dry out and irritate the skin.
- Do not remove earrings for at least 6–8 weeks (for lobe piercings) to prevent the holes from closing.
- Rotate the earrings gently while cleaning to prevent them from sticking to the skin.
- Watch for signs of infection (redness, swelling, pus, or pain) and consult a doctor if necessary.
5. Risks & Potential Complications
- Infections can occur if proper hygiene is not maintained.
- Keloids or scars can develop, especially in children with darker skin tones who are more prone to them.
- Allergic reactions can occur if non-hypoallergenic metals are used.
- Earring loss or choking hazard—for babies and toddlers, ensure earrings are secure to avoid accidental swallowing.
6. When to Seek Medical Attention
- If the ear becomes excessively swollen, painful, or has discharge.
- If the child develops a fever.
- If the earring becomes embedded in the ear.
Final Thoughts
Ear piercing can be a safe and enjoyable experience for children with proper care. Parents should weigh the pros and cons, ensure a sterile procedure, and follow aftercare instructions carefully to prevent complications.