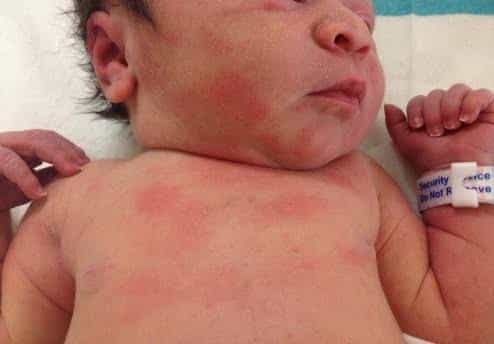
Seborrheic (seborrhoeic) dermatitis in infants, commonly called “cradle cap,” is a very common, usually harmless scaly rash that starts in the first few weeks of life and typically clears up by 6–12 months without long‑term problems.
What it is and where it occurs
It usually appears as greasy, yellow or white scales on the scalp, brows, forehead, or behind the ears (cradle cap).
It can also involve the neck folds, armpits, groin, or diaper area, often as red, shiny patches that may look like napkin dermatitis.
What parents should know
It is not an infection or poor hygiene; it is linked to overactive oil glands and the yeast Malassezia on the skin.
The baby is usually not itchy or uncomfortable, though some parents are worried about the appearance.
It is not contagious and most cases clear up on their own within weeks to months.
Home care tips for parents
Gently massage the scalp with a soft brush or washcloth after applying a small amount of mineral oil or petroleum jelly to loosen scales, then wash with a mild baby shampoo once a day.
For folds and face, keep the area clean and dry; use a fragrance‑free emollient rather than cosmetic “sensitive‑skin” products that may irritate.
When to seek medical advice
If the rash becomes very red, hot, weepy, or smelly, especially in skin folds or the diaper area, as this may indicate yeast or bacterial infection needing specific creams.
If scaling is very thick, widespread, or persists beyond 12 months, a doctor may add a low‑strength topical antifungal or steroid preparation for a short time.