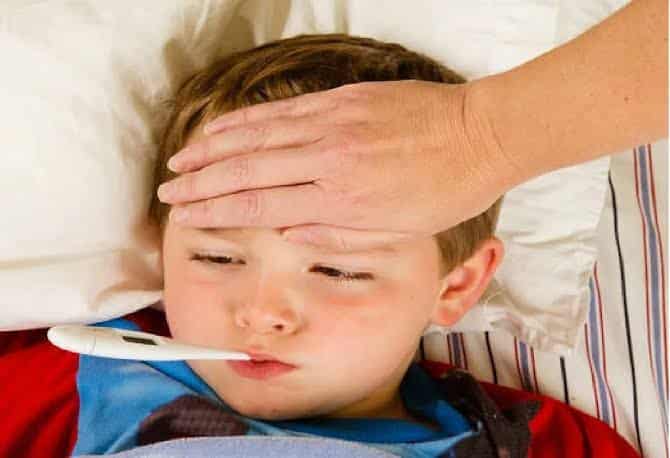
Parents in Delhi can protect children during severe heat waves by focusing on hydration, timing outdoor activities, and creating cool indoor spaces, especially amid rising temperatures like those in April 2026. These steps are critical for young kids like your 7- and 11-year-olds, who are more prone to dehydration and heat illness due to less efficient sweating.
Hydration Strategies
Encourage frequent sips of water or oral rehydration solutions throughout the day, even before thirst sets in—aim for clear urine as a sign of good hydration. Avoid sugary drinks, caffeine, or carbonated sodas, which worsen dehydration. Offer water-rich fruits like watermelon or cucumber as snacks.
Timing and Activity Limits
Keep children indoors from 11 AM to 4 PM when heat peaks; schedule play, school sports, or outings for early morning or evening. Limit strenuous activities, opting for light indoor games, and never leave kids in parked cars, even briefly. Gradually acclimate to heat over days if needed.
Clothing and Environment
Dress in loose, light-colored cotton clothes; apply broad-spectrum SPF 30+ sunscreen and hats for any sun exposure. Use fans, AC, or wet towels to cool rooms—close curtains to block sunlight—and give cool baths or showers for relief. Monitor for early signs like fatigue or dizziness.
Monitoring and Response
Watch for flushed skin, rapid breathing, headaches, or irritability, acting fast with shade, cooling, and medical help if symptoms escalate. For Delhi families, combine with your pollution guidelines: shorten outdoor time on high AQI days too. Regular rest breaks prevent fatigue from compounding heat stress.