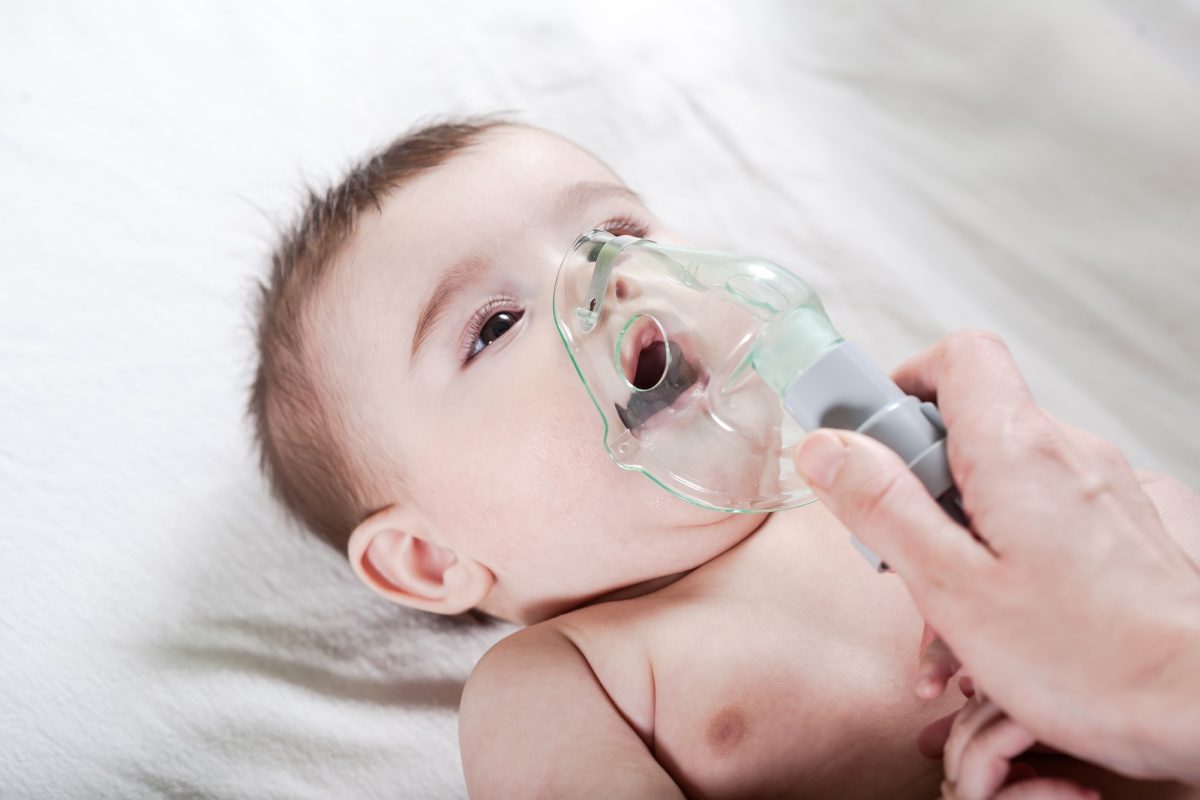
Influenza (flu) infection in infants can lead to serious illness, so it is essential for parents to understand the risks, recognize symptoms early, and know prevention and treatment measures.
Why Infants Are at Risk
Infants have a developing immune system, making them more vulnerable to severe illness from the flu compared to older children and adults.
Babies under 6 months cannot receive the flu vaccine themselves, but those 6 months and older should get vaccinated annually.
Adults and older children in close contact with infants should also be vaccinated to help protect the baby (cocooning).
How Influenza Spreads
The virus spreads through droplets in the air when an infected person coughs, sneezes, or talks.
Contact with contaminated surfaces, toys, or hands is another route; infants often touch their faces or put objects in their mouths.
Signs and Symptoms
Fever (may be high or unexplained in newborns)
Cough, runny nose, or sore throat
Unusual tiredness, irritability, or refusing to feed
Body aches, chills, or headache
Vomiting and diarrhea (more common in young children)
Severe signs: difficulty breathing, dehydration (few wet diapers), persistent high fever, or lethargy
When to Seek Medical Attention
Immediate medical attention is needed for breathing problems, bluish lips, poor feeding, dehydration, persistent vomiting, or seizures.
Consult a healthcare provider if symptoms worsen, don’t improve after a few days, or if the child appears very unwell.
Prevention Tips
Annual flu vaccination for children 6 months and older is crucial.
Vaccinate household members and caregivers if the infant is under 6 months.
Practice good hand hygiene, respiratory etiquette (cover coughs and sneezes), and disinfect surfaces regularly.
Avoid contact with people who are sick.
Keep infants away from crowded places during peak flu season.
Treatment and Home Care
Antiviral medications (e.g., oseltamivir) may be prescribed for infants at high risk or with confirmed influenza, especially if started within 48 hours of symptom onset.
Manage fever with doctor-approved medications. Do not give aspirin to infants due to the risk of Reye’s syndrome.
Keep the infant hydrated, allow rest, and monitor for worsening symptoms.
Other Key Points for Parents
Breastfeeding is encouraged; if the mother has flu symptoms, milk can be expressed and fed by a healthy caregiver.
The flu shot does not cause the flu. Some infants may have mild side effects like low-grade fever after vaccination.
Infants should stay home and away from daycare or gatherings until fever-free for at least 24 hours without fever-reducing medications.
Parents play a vital role in protecting infants from influenza by maintaining vaccination schedules, enforcing hygiene, and seeking prompt care when needed.
Parents should avoid several common mistakes when caring for a child with high fever, as these can worsen symptoms or pose risks to health.
Key Actions to Avoid
Do Not Overdress or Overcover
Heavy clothing and thick blankets trap heat and can make fever worse; always use light clothing and a thin sheet.
Never Use Rubbing Alcohol, Ice Water, or Cold Baths
Rubbing alcohol can result in poisoning through skin absorption; ice water or cold baths can trigger chills and raise body temperature instead of lowering it.
Do Not Give Aspirin
Aspirin can cause Reye syndrome, a rare but potentially fatal condition in children with viral illnesses; stick to acetaminophen or ibuprofen but never aspirin.
Avoid Forcing Food or Excessive Fluids
Do not force-feed children who have lost appetite; offer food and fluids, but let them eat what they can comfortably tolerate.
Do Not Use Spicy Foods, Tea, or Very Cold Drinks
Spices and tea can raise body temperature and irritate the digestive tract, while very cold drinks can worsen discomfort.
Do Not Combine Multiple Fever-Reducers or Flexible-Dosing
Overmedicating or using different fever reducers simultaneously can cause harmful side effects and overdose risk.
Other Common Mistakes
Do not focus only on fever; always watch for other symptoms (like rash, repetitive vomiting, or lethargy) and seek medical care as needed.
Do not use inaccurate thermometers or fail to check temperature precisely; always confirm fever with an accurate device.
Never put objects in a child’s mouth during a seizure caused by fever; this can lead to choking or injury—focus on proper seizure first aid.
When to Seek Medical Attention
Never delay seeking a doctor’s help if a child is younger than 3 months with any fever, or if a fever persists, is very high, or is accompanied by concerning symptoms like dehydration or convulsions.
These precautions help ensure safe and supportive care during childhood fevers, preventing avoidable complications and promoting recovery.
What is Typhoid Fever?
Typhoid fever is a serious bacterial infection caused by Salmonella typhi. It spreads through contaminated food and water, especially in areas with poor sanitation.
⚠️ Common Symptoms in Children:
High, sustained fever (often 102–104°F / 39–40°C)
Weakness, tiredness
Abdominal pain or discomfort
Poor appetite
Headache
Diarrhea or constipation
Coated tongue
Rash (rose spots) – flat, rose-colored spots on chest/abdomen (less common in children)
🧪 When to Suspect Typhoid:
Seek medical attention if your child has:
A fever >3 days with no clear cause
Travel history to or living in a high-risk area
Known exposure to someone with typhoid
🩺 Diagnosis:
Blood tests: Widal test, TyphiDot, or blood culture (most accurate)
Stool/urine culture (sometimes used)
💊 Treatment:
Antibiotics prescribed by a doctor (complete the full course)
Hydration and nutrition are key
Avoid over-the-counter medicines unless advised
⚠️ Warning Signs (Seek urgent care):
Vomiting everything
Altered consciousness
Severe weakness
Abdominal distension
Bleeding from nose/gums
Blood in stool
🛡️ Prevention Tips:
Typhoid vaccine (available for children above 6 months–2 years depending on vaccine type)
Safe drinking water (boiled, bottled, or filtered)
Proper handwashing before eating and after using the toilet
Avoid:
Street food
Raw fruits/vegetables not washed properly
Unpasteurized milk or dairy
🕒 How long does it last?
With treatment: Usually 7–14 days
Without treatment: Can last 3–4 weeks or lead to complications
✅ Summary for Parents:
Typhoid is preventable and treatable
Maintain good hygiene and sanitation
Complete the antibiotic course
Watch for complications
Get your child vaccinated if living in or visiting an endemic area
Fast breathing in an infant can be a normal response or a sign of an underlying health problem. Here’s what parents should know to recognize when it’s a concern and when to seek help.
🚼 What Is Normal Breathing in Infants?
Newborns (0–2 months): 30–60 breaths per minute
Infants (2–12 months): 20–50 breaths per minute
Note: Infants often breathe irregularly, with occasional pauses or bursts of rapid breathing (especially during sleep). This is usually normal.
⚠️ When Fast Breathing Might Be a Concern
Fast breathing (tachypnea) can signal several conditions, especially if it comes with other symptoms:
✅ Common Causes (Non-emergency):
Crying or fussing
Fever: Increased body temperature can increase breathing rate.
Recent feeding: Some babies breathe faster briefly after eating.
🚨 Concerning Causes:
Respiratory infections (e.g., bronchiolitis, pneumonia)
Asthma (less common in very young infants)
Congenital heart disease
Sepsis or serious infections
Metabolic disorders
🚨 When to Seek Medical Help Immediately
Call your doctor or go to the ER if your baby has:
Breathing rate consistently over 60 breaths/min
Nostrils flaring while breathing
Grunting sounds during exhalation
Chest retractions (ribs or sternum pulling in with each breath)
Bluish lips, tongue, or skin
Poor feeding
Lethargy or difficulty waking
Persistent cough, wheezing, or high-pitched sounds when breathing
👩⚕️ What a Doctor Might Do
Check oxygen levels with a pulse oximeter
Listen to lungs and heart
Order a chest X-ray or lab tests
Monitor for dehydration or signs of infection
🏠 What You Can Do at Home
Keep baby calm: crying can increase breathing rate
Track symptoms: note when it started, how fast they’re breathing, and any other signs
Keep baby upright: this may ease breathing
Avoid smoke exposure and sick contacts
Summary
Fast breathing in an infant isn’t always a medical emergency, but trust your instincts—if your baby seems unwell or you’re unsure, get checked promptly.
Cephalhematoma in a Newborn is a collection of blood between a newborn’s skull bone and the periosteum (the membrane covering the bone). It occurs due to rupture of blood vessels during delivery, often from pressure on the baby’s head during labor or use of delivery instruments like forceps or vacuum extractors.
Key Features:
Location: Always confined to one cranial bone, most commonly the parietal bone.
Does not cross suture lines (a distinguishing feature from caput succedaneum).
Appears several hours after birth, not immediately.
Firm, well-defined swelling on the head.
Skin over the swelling is not discolored, unlike in bruises.
Causes:
Birth trauma from:
Vaginal delivery
Prolonged labor
Instrumental delivery (forceps or vacuum)
Large baby (macrosomia)
Diagnosis:
Clinical examination is usually sufficient.
Imaging (ultrasound or CT) is rarely needed unless complications or other skull injuries are suspected.
Course and Management:
Benign and self-limiting — most resolve on their own over weeks to months.
No aspiration is recommended due to risk of infection.
Monitor for complications like:
Hyperbilirubinemia (due to breakdown of blood in the hematoma)
Anemia (rare)
Infection (very rare)
Caring for a crying newborn at night can be exhausting and stressful, especially for new parents. Here’s what parents should know and consider when dealing with nighttime crying:
1. Understand Why Newborns Cry
Crying is a newborn’s primary way to communicate. At night, they may cry because of:
Hunger – Newborns have small stomachs and need to feed every 2–4 hours.
Dirty diaper – A wet or soiled diaper can make them uncomfortable.
Gas or colic – Some babies have digestive discomfort or colic, causing prolonged crying.
Temperature – They may be too hot or too cold.
Sleep issues – They may be overtired or unable to self-soothe.
Need for comfort – Some babies just need to be held or feel secure.
Medical issues – If the crying is excessive and nothing helps, consult a doctor to rule out illness.
2. Tips for Soothing a Crying Newborn at Night
Feed if hungry – Watch for hunger cues (rooting, sucking motions).
Change diapers frequently – Especially before or after feeds.
Swaddle safely – This can help them feel secure.
Use white noise – A white noise machine can mimic womb sounds.
Rock or hold – Gentle rocking or holding close can comfort them.
Check for gas – Burp after feeds and consider gentle tummy massages or bicycle leg movements.
Maintain a calm environment – Dim lights, soft voices, and minimal stimulation at night help reinforce day-night cues.
3. Safe Sleep Guidelines
Always follow safe sleep practices to reduce the risk of complications
Back to sleep – Always place baby on their back to sleep.
Firm mattress – No soft bedding, pillows, or toys in the crib.
Room-sharing, not bed-sharing – Keep baby’s crib or bassinet in your room for at least 6 months.
4. Take Care of Yourself Too
Rest when you can – Sleep during baby’s naps if possible.
Share duties – If possible, rotate night shifts with a partner or family member.
Ask for help – Don’t hesitate to reach out to friends, family, or professionals.
5. When to Call the Doctor
Seek medical advice if:
The baby has a fever (especially under 3 months old).
Crying is high-pitched, nonstop, or sounds painful.
They’re not feeding well or seem lethargic.
You sense something isn’t right – always trust your instincts.
Dry skin in children is common and can result from various factors, including environmental conditions, genetics, and certain health conditions. Here’s what parents should know:
Causes of Dry Skin in Children:
- Weather: Cold, dry air in winter can strip moisture from the skin.
- Frequent Bathing: Overbathing, especially with hot water or harsh soaps, can lead to dryness.
- Genetics: Children with a family history of eczema or other skin conditions may be more prone to dry skin.
- Dehydration: Not drinking enough water can contribute to dry skin.
- Skin Conditions: Conditions like eczema or psoriasis can cause dry, flaky skin.
Symptoms:
- Rough, scaly, or flaky skin.
- Itching or discomfort.
- Red or irritated patches.
- Cracks or peeling, especially on hands, feet, or lips.
Prevention and Care Tips:
- Moisturize Regularly: Apply a thick, fragrance-free moisturizer immediately after bathing and several times a day as needed.
- Limit Bath Time: Keep baths or showers short and use lukewarm water. Avoid hot water, which can dry out the skin.
- Use Gentle Cleansers: Opt for mild, fragrance-free soaps or cleansers specifically designed for children’s sensitive skin.
- Humidify the Air: Using a humidifier in the child’s room can help maintain moisture levels in the air, especially in winter.
- Dress Appropriately: Dress children in soft, breathable fabrics like cotton. Avoid wool or synthetic materials that may irritate the skin.
- Hydration: Ensure the child drinks plenty of water to keep the skin hydrated from the inside.
- Sun Protection: Use a broad-spectrum sunscreen to protect the skin from drying and damaging UV rays.
When to See your paediatrician:
- If the dry skin is persistent, severe, or accompanied by symptoms like redness, swelling, or oozing.
- If the child develops signs of infection (e.g., redness, warmth, or pus).
- If you suspect eczema or another skin condition that may require specific treatment.
Proper skincare and preventive measures can help manage and reduce the occurrence of dry skin in children.
If a child is choking, it’s important to act quickly. Here’s what parents or caregivers should do:
1. Assess the Situation
- Mild choking: The child may cough or make wheezing sounds. If they are still able to breathe and cough, encourage them to keep coughing to clear the obstruction.
- Severe choking: The child may not be able to breathe, cry, or cough. Their face may turn red or blue. Immediate action is needed.
2. For Infants (Under 1 Year Old)
If the infant is choking and unable to cough or breathe:
- Call for help (call emergency services if needed).
- Perform back blows:
- Place the infant face-down on your forearm, supporting the head and neck.
- Use the heel of your hand to give up to 5 back blows between the infant’s shoulder blades.
- Perform chest thrusts:
- If the back blows don’t clear the obstruction, turn the infant over to face-up.
- Place two fingers in the center of the chest just below the nipple line.
- Give 5 chest thrusts, pushing down firmly.
- Repeat the back blows and chest thrusts until the object is expelled or emergency help arrives.
3. For Children (Over 1 Year Old)
If the child is choking and unable to breathe:
- Call for help (call emergency services if needed).
- Perform back blows:
- Have the child bend forward at the waist.
- Use the heel of your hand to give 5 firm back blows between the shoulder blades.
- Perform abdominal thrusts (Heimlich maneuver):
- Stand behind the child and place your hands around their waist.
- Make a fist with one hand and place the thumb side just above the child’s navel.
- Grasp the fist with your other hand and give quick inward and upward thrusts.
- Continue the thrusts until the object is expelled or the child begins to breathe.
4. After the Object Is Expelled
- If the child begins breathing, stay with them and monitor for any further complications.
- If the child is still not breathing, begin CPR and continue until help arrives.
5. Do Not
- Do not slap the child on the back or try to retrieve the object with your fingers unless you can clearly see it and can easily remove it without pushing it deeper.
- Do not perform abdominal thrusts on infants.
It’s crucial to take immediate action, and if you’re unsure, always call emergency services for professional guidance.
Frequent urination in toddlers can have various causes, and it’s important to pay attention to any accompanying symptoms. Here are some common reasons:
- High Fluid Intake: If your toddler is drinking more fluids than usual, they may urinate more frequently. This is usually harmless and can be adjusted by limiting fluid intake before bedtime or during certain times of the day.
- Bladder Infection (UTI): A urinary tract infection can cause frequent urination, often accompanied by discomfort or pain, changes in urine color (e.g., cloudy or blood-tinged), and sometimes fever. If you suspect a UTI, a doctor can perform tests to confirm it.
- Diabetes: Unexplained frequent urination, especially if combined with excessive thirst, could be a sign of diabetes. This is rare in toddlers but can be tested with blood work.
- Constipation: Constipation can put pressure on the bladder, leading to frequent urination. If your toddler is also struggling with bowel movements, this may be the cause.
- Normal Development: Some toddlers just have smaller bladders or may still be adjusting to their potty training routines, leading to more frequent trips to the bathroom.
- Psychological Factors: Stress or anxiety (e.g., starting preschool or a change in routine) can sometimes cause frequent urination.
If you’re concerned about the frequency of urination or if your toddler shows signs of discomfort, pain, or other symptoms, it’s best to consult a pediatrician for further evaluation.