Identifying infections in newborns can be challenging because their immune systems are not fully developed, and their symptoms may not always be obvious. However, there are several key signs parents can watch for to detect potential infections early. Here are some tips to help:
1. Watch for Fever
- Fever (or low temperature): A temperature above 100.4°F (38°C) or below 97.5°F (36.4°C) could indicate an infection. In newborns, even a low fever can be a sign of serious illness and in most cases fever might not be present.
2. Monitor Feeding Habits
- Difficulty feeding: If your baby suddenly loses interest in feeding or has difficulty breastfeeding or bottle-feeding, this may be a red flag.
- Vomiting or frequent spit-ups: Though some spit-up is normal, persistent vomiting can be a sign of an infection, especially if it’s accompanied by other symptoms.
3. Observe Breathing Patterns
- Labored or rapid breathing: Fast breathing (more than 60 breaths per minute), grunting sounds, or pauses in breathing may indicate respiratory distress or infection.
4. Check for Changes in Skin Color
- Pale, bluish, or mottled skin: This can be a sign of poor oxygenation or circulation, possibly due to infection.
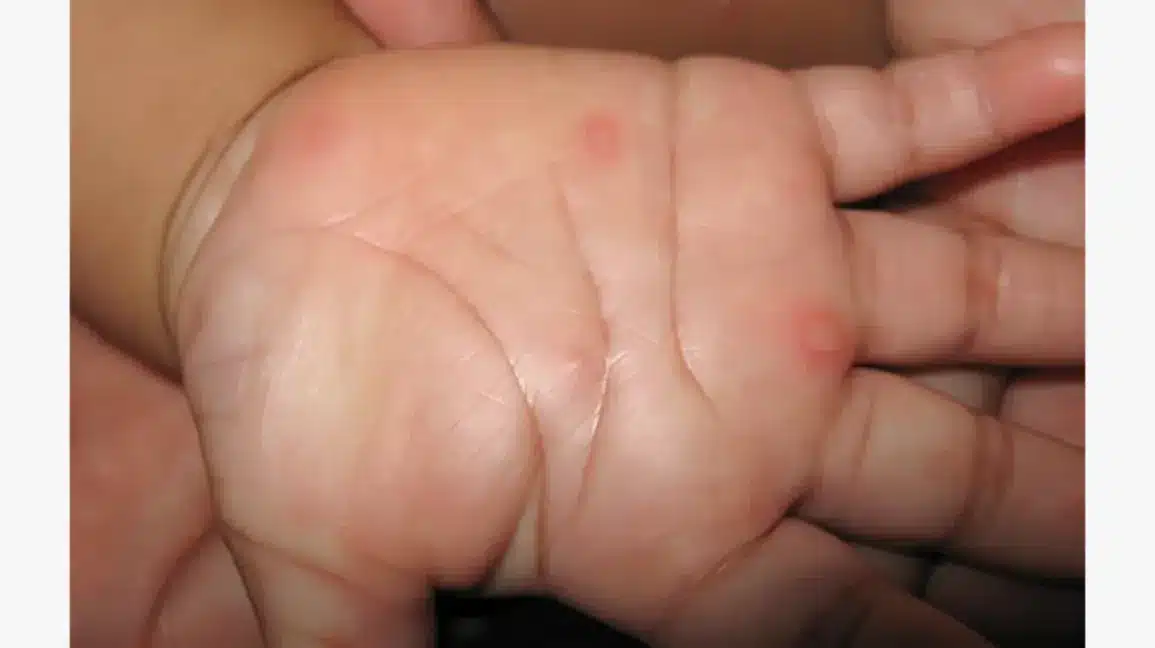
- Rashes: While some newborn rashes are normal, a sudden onset of an unusual rash, especially one that doesn’t fade with pressure, could signal an infection.
5. Track Diaper Changes
- Decreased urination: Fewer wet diapers than usual may indicate dehydration, which could be a sign of an infection.
- Diarrhea: Watery, foul-smelling stools or a sudden increase in stool frequency might indicate a gastrointestinal infection.
6. Look for Behavioral Changes
- Excessive fussiness or irritability: While crying is normal for newborns, constant crying, especially if it’s out of the ordinary, may signal discomfort from an infection.
- Lethargy or decreased activity: If your baby seems unusually sleepy, weak, or difficult to wake, this could indicate an infection.
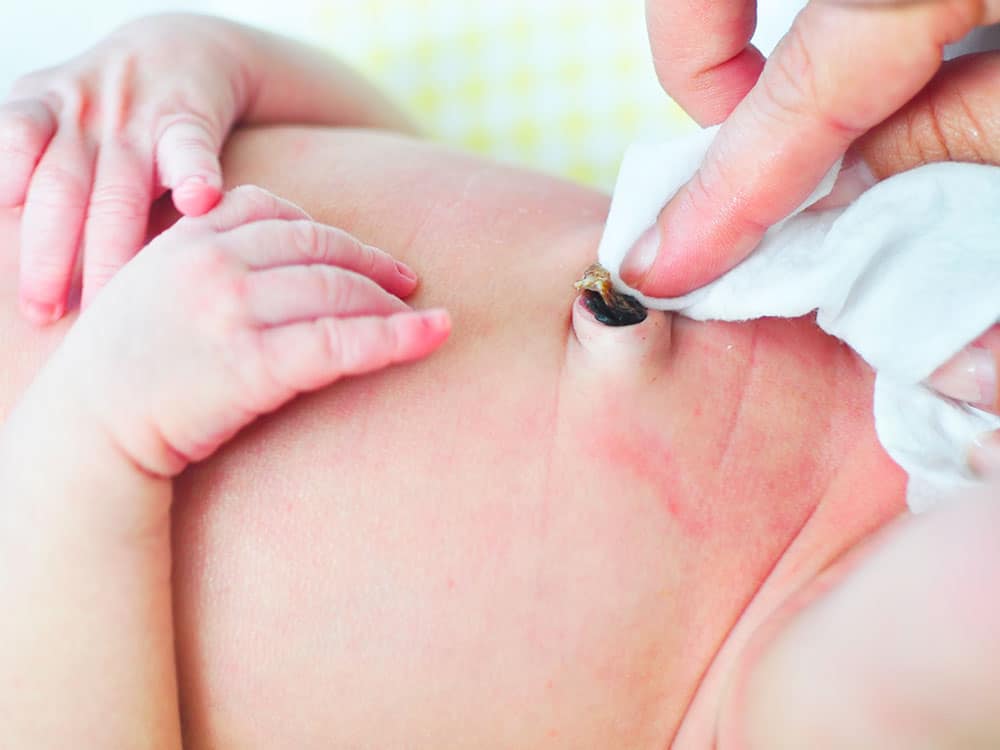
7. Check the Umbilical Cord or Circumcision Site
- Redness, swelling, or discharge: Any sign of infection around the umbilical cord stump or circumcision site (if applicable), such as pus or a bad smell, needs medical attention.
8. Monitor Jaundice
- Prolonged or worsening jaundice: Yellowing of the skin and eyes is common in newborns but should improve after a few days. If it worsens or persists, it could indicate an underlying infection or liver issue.
9. Unusual Crying Sounds
- High-pitched or weak cry: A cry that sounds different from your baby’s normal cry may indicate discomfort or illness.
10. Seek Medical Attention
- Trust your instincts: If something doesn’t seem right, it’s always best to consult your pediatrician. Newborn infections can escalate quickly, so early detection and treatment are critical.
If you observe any of these signs, particularly in combination, it’s essential to contact your pediatrician promptly.