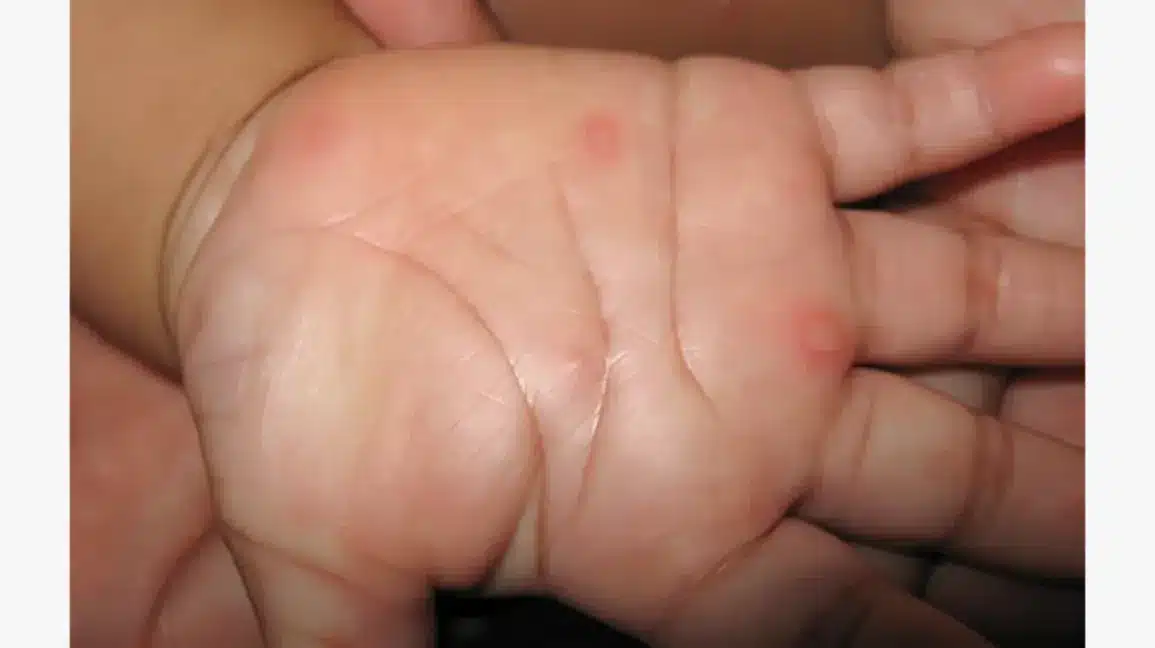
Excess oil usage in newborns can lead to several issues:
- Skin Irritation: Newborn skin is delicate and can be easily irritated. Excessive oil can clog pores and lead to rashes or acne.
- Allergic Reactions: Some oils may cause allergic reactions, leading to redness, swelling, or discomfort.
- Impaired Skin Barrier: Overuse of oil can disrupt the natural moisture balance and skin barrier function, making the skin more vulnerable to infections.
- Heat Rash: Oils can trap heat, potentially causing heat rash or increased discomfort in warm environments.
- Dirt and Bacteria Build-Up: Excess oil can attract dirt and bacteria, increasing the risk of infections.
For newborns, it’s usually best to use minimal products and consult a pediatrician before applying any oils.