Managing high fever in children can be distressing for parents. Here are some valuable parental tips:
Assessment
1. Check temperature: Use a digital thermometer preferably axillary temperature.
2. Observe behavior: Monitor for signs of distress, irritability, or lethargy.
Home Management
1. Fluids: Encourage oral fluids (breast milk, formula, or any liquids).
2. Medication:
– Acetaminophen/paracetamol (crocin/ calpol/ t-98 etc): consult pediatrician for dosage.
– Avoid other medicines like meftal (mefenemic acid) or brufen (ibuprofen) unless prescribed by your pediatrician.
3. Dressing: Dress child lightly to promote heat loss.
4. Bathing: Sponge baths with lukewarm water (not cold water).
5. Rest: Encourage quiet activities.
When to Seek Medical Attention
1. Fever >104°F (40°C) in children <3 months.
2. Fever >102°F (39°C) in children 3-6 months.
3. Fever lasting >72 hours.
4. Signs of dehydration (dry mouth, fewer wet diapers).
5. Difficulty breathing, headache, stiff neck.
6. Vomiting, diarrhea, or abdominal pain.
7. Rash, seizure, or altered mental status.
Additional Tips
1. Monitor for fever spikes.
2. Use fever-reducing medications only as directed.
3. Avoid:
– Aspirin in children <18 years.
– Cold or ice baths.
– Overdressing.
– Overmedicating.
4. Maintain vaccinations to prevent fever-causing illnesses.
Red Flags
1. Infant <3 months with fever.
2. Fever with petechiae (small, purple spots).
3. Fever with difficulty breathing.
4. Severe headache or stiff neck.
5. Altered mental status or confusion.
Consult your pediatrician for personalized advice and guidance.
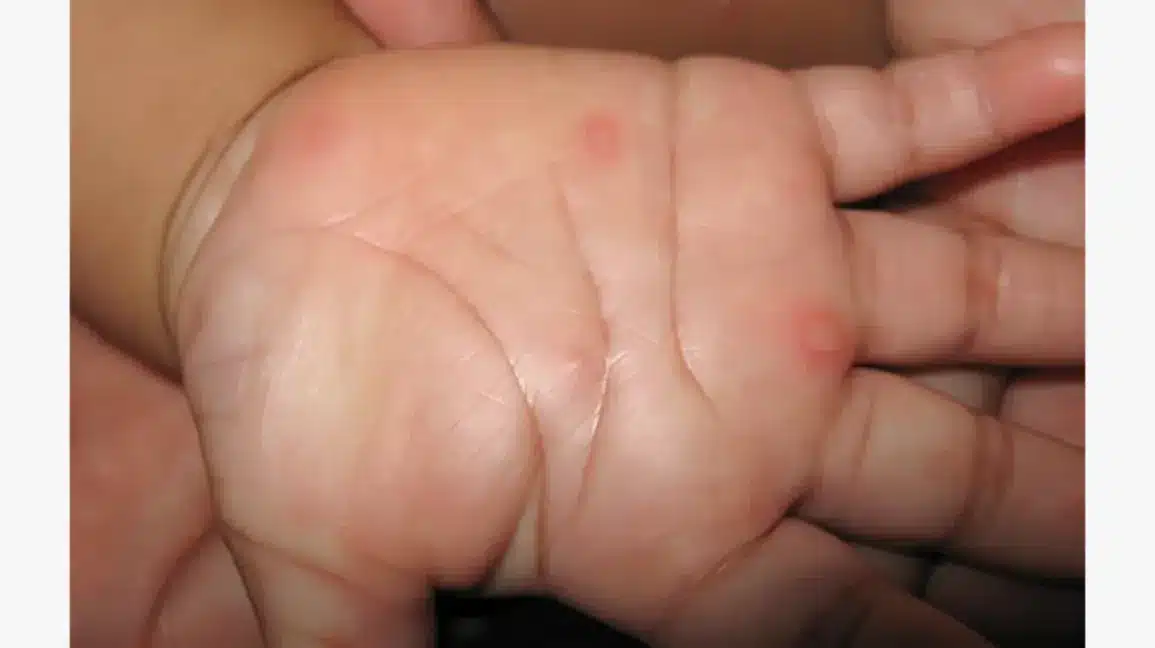
Hand, Foot, and Mouth Disease (HFMD) is a contagious viral infection common in young children. It typically causes fever, sores in the mouth, and a rash on the hands and feet. If your child has HFMD, here are some precautions parents should take:
1. Practice Good Hygiene:
- Handwashing: Wash hands frequently with soap and water, especially after changing diapers, using the bathroom, and before preparing food.
- Avoid Touching Face: Try to avoid touching your eyes, nose, and mouth without washing your hands first.
- Disinfect Surfaces: Regularly clean and disinfect frequently touched surfaces, such as toys, doorknobs, and countertops.
2. Isolation:
- Keep Your Child Home: If your child is diagnosed with HFMD, keep them home from school or daycare until they are fever-free and sores have healed, which typically takes about 7–10 days.
- Avoid Close Contact: Avoid kissing, hugging, and sharing utensils with the infected child to reduce the spread of the virus.
3. Monitor Symptoms:
- Fever and Pain Management: Use over-the-counter pain relievers like acetaminophen or ibuprofen to manage fever and discomfort.
- Hydration: Ensure your child stays hydrated. Offer plenty of fluids, but avoid acidic drinks that might irritate mouth sores.
4. Seek Medical Attention:
- Complications: If your child is unable to swallow, shows signs of dehydration (like reduced urination), or has a high fever, seek medical attention promptly.
- Follow-Up: Keep in touch with your pediatrician if symptoms worsen or don’t improve as expected.
5. Educate Others:
- Inform Caregivers: Let any other caregivers or family members know about the infection and the necessary precautions.
- Community Awareness: Notify your child’s school or daycare so they can take appropriate measures to prevent further spread.
By following these precautions, you can help reduce the spread of HFMD and ensure your child’s comfort during recovery.
Ensuring that children get proper sleep is crucial for their physical and mental development. Here are some key points parents should know:
1. Recommended Sleep Duration
- Newborns (0-3 months): 14-17 hours per day
- Infants (4-11 months): 12-15 hours per day
- Toddlers (1-2 years): 11-14 hours per day
- Preschoolers (3-5 years): 10-13 hours per day
- School-age children (6-13 years): 9-11 hours per day
- Teenagers (14-17 years): 8-10 hours per day
2. Consistent Sleep Schedule
- Maintain regular bedtimes and wake-up times, even on weekends.
- Consistency helps regulate the body’s internal clock.
3. Creating a Sleep-Conducive Environment
- Keep the bedroom dark, cool, and quiet.
- Limit exposure to screens (TVs, tablets, phones) at least an hour before bed, as the blue light can interfere with melatonin production.
4. Bedtime Routine
- Establish a calming bedtime routine, such as reading a book, taking a bath, or listening to soft music.
- Routines signal to the body that it’s time to wind down.
5. Diet and Nutrition
- Avoid heavy meals, caffeine, and sugary foods close to bedtime.
- A light snack before bed is okay, but it should be nutritious and not too filling.
6. Physical Activity
- Encourage regular physical activity during the day, but avoid vigorous exercise close to bedtime.
7. Addressing Sleep Issues
- If a child has trouble falling or staying asleep, it may be helpful to track their sleep patterns and consult a pediatrician.
- Common issues include nightmares, night terrors, sleepwalking, and sleep apnea.
8. Understanding Developmental Changes
- Be aware that sleep needs and patterns can change with age and developmental stages.
- For teenagers, biological changes can lead to a natural shift in sleep-wake cycles, making them prone to staying up later and waking up later.
9. Encouraging Independence
- For younger children, encourage self-soothing techniques to help them fall back asleep on their own if they wake up during the night.
10. Modeling Good Sleep Habits
- Children often mimic their parents’ behaviors, so it’s essential for parents to model good sleep hygiene.
Good sleep is vital for children’s growth, learning, and overall well-being. If parents have concerns about their child’s sleep, consulting your pediatrician is advisable.
Colic is a common condition in infants, characterized by episodes of intense, unexplained crying and discomfort. It typically occurs in the first few months of life and can be very distressing for both the baby and the parents. Here’s what parents need to know about colic pain in infants:
Symptoms of Colic:
- Intense Crying: Episodes of crying that last for several hours, usually occurring in the late afternoon or evening.
- Clenched Fists: The baby may clench their fists, curl their legs, and tense their abdominal muscles.
- Facial Grimacing: The baby might have a pained expression and may appear to be in distress.
- Difficulty Sleeping: Colicky babies often have trouble falling asleep or staying asleep.
Possible Causes:
The exact cause of colic is unknown, but several factors may contribute:
- Digestive Issues: Immature digestive systems may lead to gas, bloating, and discomfort.
- Overstimulation: Sensory overload from lights, sounds, and activities can contribute to colic.
- Feeding Problems: Difficulty feeding, whether breastfeeding or bottle-feeding, can sometimes cause colic symptoms.
- Allergies or Intolerances: In some cases, food allergies or intolerances (such as to cow’s milk) may be a factor.
Management and Relief Strategies:
- Comforting Techniques: Rocking, swaddling, holding the baby, or using a pacifier can provide comfort.
- Burping: Ensure the baby is burped frequently during and after feedings to reduce gas.
- Warm Baths: A warm bath can sometimes soothe a colicky baby.
- Probiotics: Some studies suggest that probiotics may help reduce colic symptoms in breastfed babies.
- Dietary Changes:For formula-fed babies, trying a different formula may be beneficial.
- Holding Positions: Holding the baby in different positions, such as upright or on their stomach across your forearm, may provide relief.
When to Seek Medical Advice:
- Severe or Prolonged Crying: If the crying is exceptionally severe or lasts for more than three hours a day, it’s important to consult a healthcare provider.
- Feeding Difficulties: If the baby is not feeding well, losing weight, or has other symptoms like vomiting or diarrhea.
- Health Concerns: Any concerns about the baby’s health or development should be discussed with a pediatrician.
Support for Parents:
- Take Breaks: It’s essential for parents to take breaks and ask for help to manage stress and fatigue.
- Parenting Groups: Joining a support group or talking to other parents can provide emotional support and practical tips.
- Professional Help: If the stress becomes overwhelming, seeking professional help from a healthcare provider or counselor is advisable.
Colic can be challenging, but it usually improves by the time the baby is about 3-4 months old. With patience, support, and appropriate management, parents can help their baby through this difficult phase.